Physician burnout remains a critical issue in modern healthcare, driven largely by an overwhelming administrative burden. Physicians now spend over three hours daily on clinical documentation alone, with an additional 1.77 hours of “pajama time” — after-hours EHR work — corroding personal well-being. This relentless clerical demand, which can consume up to 28 hours per week, is a primary factor in the staggering 43.2% of U.S. physicians who reported burnout symptoms in 2024. The consequences are severe, impacting not only clinician morale but also patient access and quality of care.
In response, AI medical scribes have transitioned from an emerging novelty to a clinical standard. These ambient AI documentation tools offer a powerful solution by passively listening to physician-patient conversations and generating structured clinical notes in real time. Unlike traditional voice dictation software that required clinicians to speak structured sentences, ambient AI understands natural, free-flowing dialogue and automatically generates SOAP notes, HPIs, and comprehensive assessment and plan sections. The impact is significant: one study found AI scribes reduced average note completion time from 8.9 minutes to just 5.1 minutes — a 43% improvement. This proven ROI has fueled rapid adoption, with over 600 healthcare organizations implementing Nuance DAX Copilot alone by 2025.
As the market accelerates, early concerns about security and compliance have been addressed by leading platforms. Today, virtually all reputable AI scribes are HIPAA-compliant, offer Business Associate Agreements (BAAs), and hold rigorous certifications like SOC 2 Type II. Data is secured through robust encryption and secure cloud processing, allowing physicians to adopt these time-saving tools with confidence. For providers drowning in paperwork, the question is no longer if they should consider an AI scribe, but which one is the right fit for their practice, specialty, and workflow.
Evaluation Criteria
- Clinical Accuracy & Note Quality: Ability to generate accurate, structured, specialty-appropriate clinical notes from ambient conversation.
- Ambient Listening vs. Active Dictation: Whether the tool works passively in the background or requires the clinician to speak structured prompts.
- EHR Integration Depth: Native Epic/Cerner/athena integrations vs. copy-paste workflows.
- Specialty Coverage: Number of supported specialties and availability of specialty-tuned templates.
- HIPAA Compliance & Security: BAA availability, data encryption, SOC 2 Type II, on-device vs. cloud processing.
- Ease of Use & Onboarding: Time to get up and running, learning curve, mobile app quality.
- Pricing & ROI: Monthly cost per provider vs. time saved and productivity gained.
- Post-Visit Workflow: After-visit summaries, patient instructions, coding suggestions, prior auth assistance.
- User Ratings: G2, Capterra, KLAS, and Software Advice verified reviews.
Top 10 AI Medical Scribe Tools
1. Nuance DAX Copilot (Microsoft)

Nuance DAX Copilot, developed by Microsoft and integrated into the Microsoft Cloud for Healthcare, is the undisputed enterprise leader in ambient AI clinical documentation. Launched initially as “Dragon Ambient eXperience,” DAX Copilot leverages Microsoft’s Azure OpenAI Service and the clinical expertise embedded in Dragon Medical to deliver one of the most accurate and deeply integrated AI documentation experiences available. As of early 2025, over 600 healthcare organizations — including major health systems like UC San Diego Health, Sutter Health, and Providence — have deployed DAX Copilot. The platform integrates with 200+ EHRs and operates directly inside the Epic SmartTools workflow, making it the gold standard for enterprise-scale deployment.
- Star Rating: 4.5 / 5
- Target Audience: Large health systems and enterprise hospital networks.
Key Features:
- Ambient AI that passively listens to patient-provider conversations and auto-generates structured SOAP notes
- Native integration with Epic (in-basket), Oracle Cerner, Meditech, and 200+ EHR systems
- Microsoft Azure OpenAI-powered large language model with continuous clinical fine-tuning
- Real-time note generation available on mobile app (iOS/Android) or web
- Supports 20+ medical specialties with specialty-specific documentation templates
- Integrated coding suggestions and charge capture support
- Enterprise-grade HIPAA compliance: SOC 2 Type II, BAA, encrypted processing
Pricing: Starts at approximately $369–$444/provider/month (enterprise contracts; pricing varies by organization size and deployment scope).
Pros:
- Unmatched EHR integration breadth — works inside Epic’s native SmartTools environment
- Backed by Microsoft’s enterprise infrastructure — highly reliable and scalable
- Proven ROI: documented 50% reduction in documentation time for many health systems
- Continuous model improvement via Microsoft’s clinical AI research investment
- Exceptional enterprise security and compliance posture
Cons:
- High cost — not accessible for solo practitioners or small practices
- Primarily designed for enterprise; smaller practices may find it overpowered for their needs
- Requires IT infrastructure support for full deployment
- Onboarding complexity is higher than consumer-grade alternatives
Best for: Large hospital systems, academic medical centers, and multi-site health networks requiring deep EHR integration and enterprise-grade security at scale.
2. Abridge
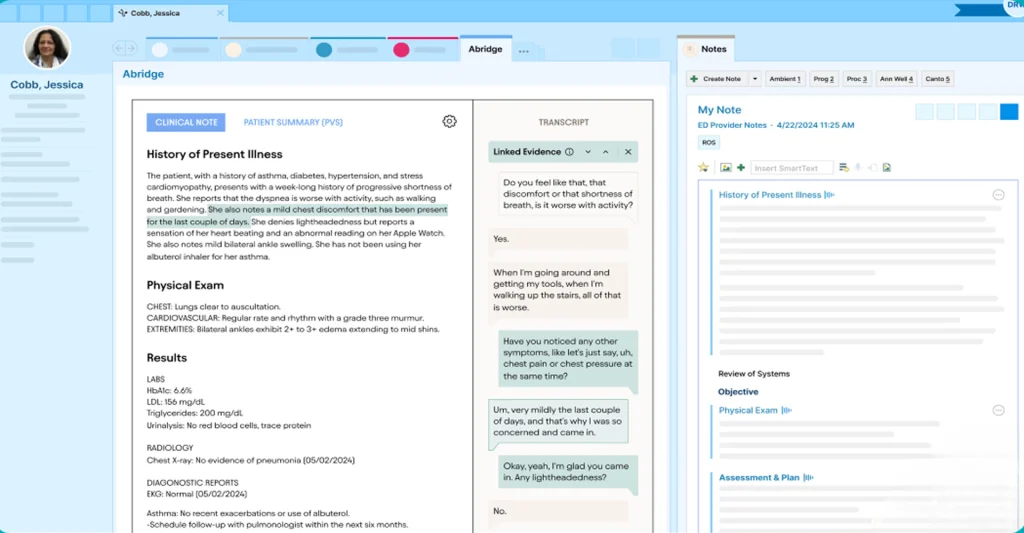
Abridge has rapidly emerged as one of the most talked-about AI medical scribe platforms in the industry, having secured a landmark partnership with the University of Pittsburgh Medical Center (UPMC) and becoming a preferred Epic-native ambient AI documentation solution. The platform supports 28 languages and covers 50+ medical specialties, making it one of the most linguistically capable ambient scribes available. Unlike many competitors, Abridge’s AI model is trained on millions of de-identified clinical conversations, giving it exceptional contextual understanding of complex medical dialogue.
- Star Rating: 4.5 / 5
- Target Audience: Epic-integrated health systems and academic medical centers.
Key Features:
- Epic-native integration — documentation generated directly within the Epic workflow
- Supports 28+ languages for multilingual patient populations
- Covers 50+ medical specialties with specialty-tuned conversation models
- Ambient AI — no structured dictation required; listens naturally to patient encounters
- Generates SOAP notes, after-visit summaries, and patient-friendly instructions
- Trained on a vast de-identified clinical conversation dataset for clinical accuracy
- Real-time and post-visit note review with one-click EHR push
Pricing: Approximately $208/provider/month (health system contracts may vary; enterprise pricing available).
Pros:
- Best-in-class multilingual support (28+ languages) — critical for diverse patient populations
- Epic-native integration reduces workflow friction significantly
- Outstanding clinical accuracy, particularly in complex multi-issue encounters
- Strong academic/research medical center adoption track record
- Excellent patient-facing after-visit summaries improve care adherence
Cons:
- Primarily optimized for Epic — less seamless on other EHR platforms
- Pricing may be higher than solo-practice budget solutions
- Enterprise-focused; limited self-serve onboarding path for small practices
Best for: Epic-based health systems, academic medical centers, and multi-specialty groups serving diverse or multilingual patient populations.
3. Ambience Healthcare
Ambience Healthcare is a full-stack ambient AI clinical documentation platform that has distinguished itself with a comprehensive, end-to-end approach to physician workflow automation. The platform does more than just generate notes — it integrates Clinical Documentation Improvement (CDI), coding assistance, quality measure tracking, and prior authorization support into a single ambient AI layer. Its platform is built on a proprietary medical language model trained specifically on clinical conversations, not general-purpose LLMs, which produces more clinically precise and contextually appropriate documentation.
- Star Rating: 4.4 / 5
- Target Audience: Enterprise health systems seeking comprehensive AI documentation and clinical intelligence.
Key Features:
- Full ambient AI documentation with real-time note generation across 100+ specialties
- Integrated Clinical Documentation Improvement (CDI) alerts within the documentation workflow
- Automated medical coding suggestions (ICD-10, CPT) to support revenue cycle
- Prior authorization drafting and quality measure documentation support
- Native integrations with Epic, Oracle Cerner, and major EHR platforms
- Proprietary medical LLM trained exclusively on clinical conversations
- HIPAA-compliant, SOC 2 Type II, with BAA available
Pricing: Enterprise pricing — contact Ambience for custom quotes (typically $400–$600+/provider/month).
Pros:
- Comprehensive platform — documentation, CDI, coding, and prior auth in one ambient AI layer
- Proprietary clinical LLM produces highly accurate, specialty-specific notes
- Strong enterprise health system deployments (Cleveland Clinic, etc.)
- KLAS recognition adds third-party validation of clinical and operational performance
- Particularly strong in complex specialties where documentation accuracy is critical
Cons:
- Enterprise-only pricing model — not viable for small or independent practices
- More complex implementation than lighter-weight consumer tools
- Longer time to full deployment compared to cloud-only SaaS alternatives
Best for: Large health systems and enterprise networks seeking a single ambient AI platform that goes beyond documentation to include CDI, coding support, and clinical intelligence.
4. Suki AI
Suki AI is one of the pioneering AI medical voice assistants, built on the premise that physicians should be able to interact with their EHR entirely through natural voice commands — not just for documentation, but for chart lookups, medication history review, and order drafting. Founded in 2017 and backed by significant venture investment, Suki has evolved from a voice-command assistant to a full ambient AI documentation platform that generates clinical notes from natural conversations. Its integrations with Epic, Oracle Health, and athenahealth, combined with a polished mobile app experience, have made it a strong choice for individual clinicians and smaller practices.
- Star Rating: 4.3 / 5
- Target Audience: Individual physicians and mid-size practices seeking a fast, voice-first AI scribe.
Key Features:
- Ambient AI documentation from natural physician-patient conversation — no structured dictation
- Voice-first EHR navigation: look up chart data, review histories, and draft orders by voice
- Native integrations with Epic, Oracle Health (Cerner), and athenahealth
- Specialty-specific note templates across primary care, cardiology, orthopedics, and more
- Mobile app (iOS/Android) supports on-the-go documentation and chart review
- Customizable note formats with physician-specific learning over time
- HIPAA-compliant with SOC 2 Type II certification and BAA
Pricing: Approximately $299/provider/month.
Pros:
- Voice-first design delivers the most natural, low-friction physician experience
- Excellent mobile app allows documentation anywhere, including telemedicine visits
- EHR navigation by voice (beyond just notes) is a unique and time-saving capability
- Strong physician-specific learning — adapts to individual documentation style over time
- Reasonable pricing for the feature set compared to enterprise alternatives
Cons:
- Voice-command EHR navigation requires more deliberate physician engagement than fully passive ambient tools
- Smaller customer base than Nuance or Abridge, with less peer-reviewed clinical evidence
- Integration breadth is narrower than enterprise competitors (primarily Epic, Oracle, Athena)
- Some users report the learning curve for voice customization can take 2–3 weeks
Best for: Individual physicians and small-to-mid-size practices using Epic, Oracle Health, or athenahealth who want a voice-first, highly personalized AI documentation experience.
5. DeepScribe
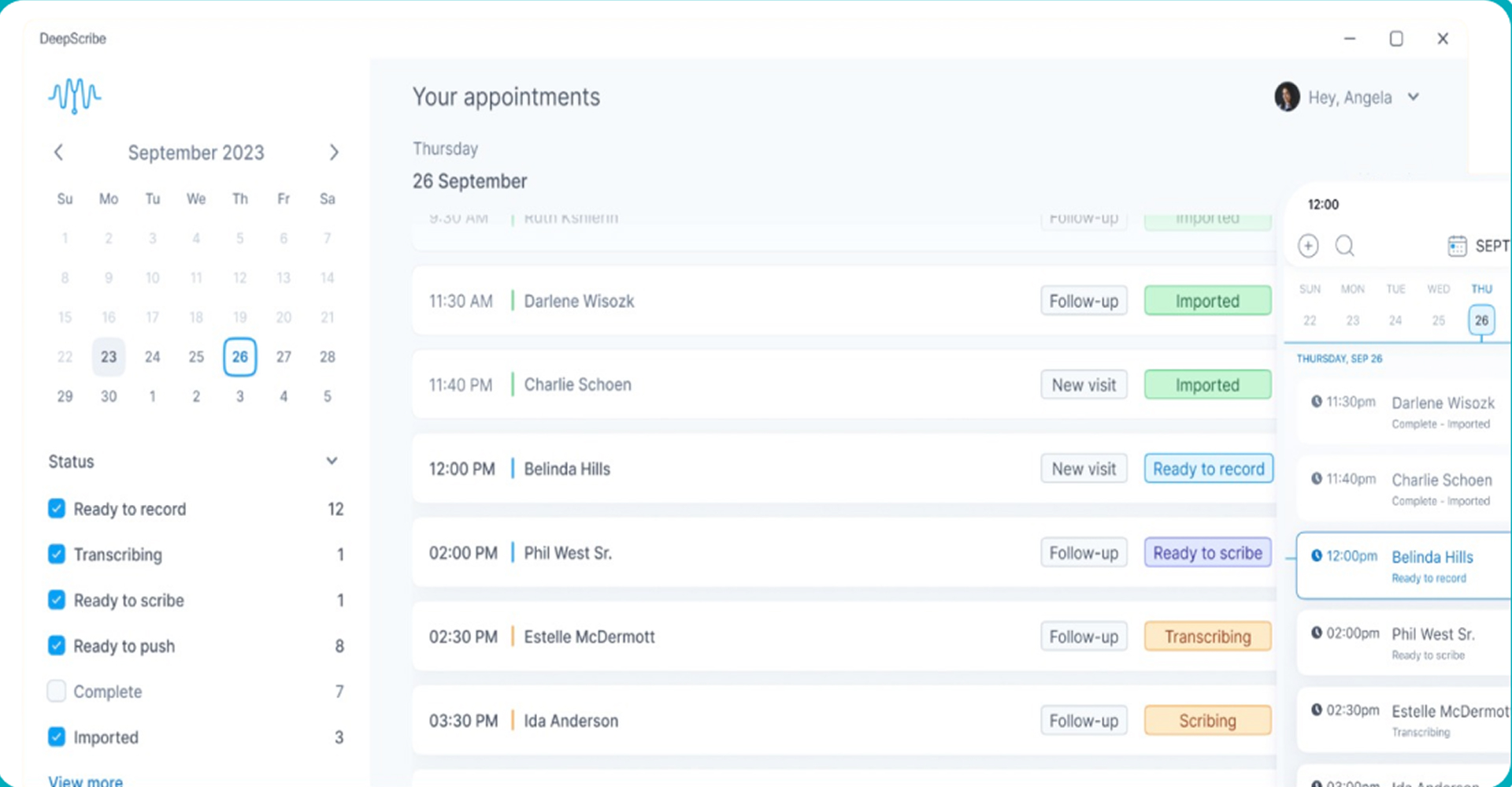
DeepScribe positions itself as the premium tier of ambient AI documentation, having built its platform with an emphasis on clinical accuracy in complex, high-acuity specialties where note quality has direct implications for billing, compliance, and patient safety. Unlike general-purpose AI scribes, DeepScribe was built from the ground up for specialists — oncologists, cardiologists, neurologists, and other high-complexity physicians who cannot afford documentation errors. The platform uses a multi-layer AI approach combining speech recognition, NLP, and a clinical knowledge graph to produce notes with a reported 99%+ accuracy rate.
- Star Rating: 4.3 / 5
- Target Audience: High-complexity specialty practices requiring the most clinically nuanced documentation.
Key Features:
- Multi-layer AI pipeline: speech recognition + NLP + clinical knowledge graph for maximum accuracy
- Purpose-built templates for high-complexity specialties (oncology, cardiology, neurology, pain management)
- Supports 50+ medical specialties with deep specialty customization
- Real-time ambient documentation — completely hands-free during the patient encounter
- Integrates with Epic, Oracle Cerner, athenahealth, Greenway, and 40+ EHR platforms
- Medical coding suggestions to support specialty billing accuracy
- HIPAA-compliant, SOC 2 Type II; all audio processing is secure and encrypted
Pricing: Approximately $750/provider/month (premium tier; reflects enterprise-grade clinical accuracy focus).
Pros:
- Best-in-class clinical accuracy, particularly for complex specialty documentation
- Multi-layer AI approach catches terminology nuances that simpler models miss
- Broad EHR integration portfolio — compatible with most platforms
- Deep specialty customization — templates built for each specialty’s documentation needs
- Strong ROI in high-volume specialty practices where billing accuracy matters most
Cons:
- Highest price point of any platform — difficult to justify for primary care or lower-volume practices
- More complex onboarding than simpler consumer tools
- Primarily optimized for specialists — may feel like overkill for straightforward primary care notes
- Some users report the note format can be verbose for simpler encounters
Best for: Oncology, cardiology, neurology, orthopedics, and other high-complexity specialty practices where documentation accuracy has direct implications for coding, compliance, and patient outcomes.
6. Freed AI
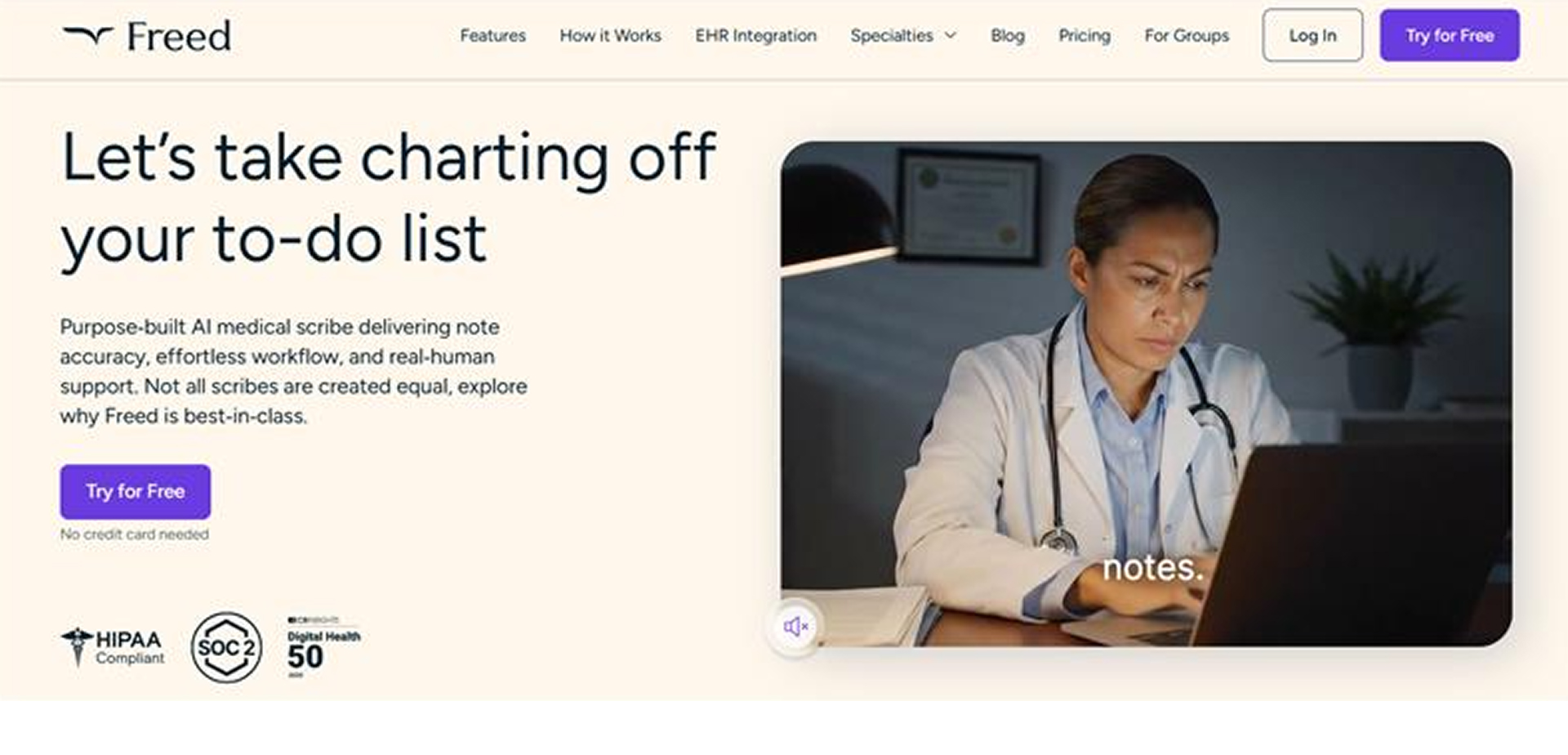
Freed AI has become the go-to AI medical scribe for solo practitioners and small practices by offering a genuinely frictionless documentation experience at a price point that makes ambient AI accessible for the first time to independent physicians. Unlike enterprise platforms that require IT deployment and long onboarding cycles, Freed works entirely through a browser-based or mobile interface — no IT setup required. A physician simply opens the app, starts the encounter, and receives a complete SOAP note within seconds of the visit ending. Freed’s AI learns each physician’s unique documentation style over time, producing increasingly personalized notes with every encounter.
- Star Rating: 4.4 / 5
- Target Audience: Independent physicians, solo practitioners, and small practices.
Key Features:
- Browser-based and mobile app (iOS/Android) — no IT installation required; works with any EHR
- Ambient listening generates complete SOAP notes automatically from physician-patient conversation
- AI-powered style learning — adapts to each physician’s documentation preferences over time
- Supports primary care, family medicine, pediatrics, OB/GYN, psychiatry, and 20+ specialties
- After-visit patient summaries and instructions generated automatically
- One-click copy-paste into any EHR (no native integration required for basic use)
- HIPAA-compliant with BAA, SOC 2 Type II, and encrypted audio processing
Pricing: $39/month (Starter), $79/month (Core), $119/month (Premier).
Pros:
- Most affordable premium ambient AI scribe on the market — accessible to solo and independent practitioners
- Zero IT setup required — start generating notes in under 10 minutes
- AI style learning produces increasingly personalized, accurate notes with use
- Flexible pricing tiers allow practices to scale without large upfront commitments
- Exceptional ease of use with minimal learning curve — widely praised in physician reviews
Cons:
- No native EHR integration in basic tier — requires manual copy-paste into the EHR
- Less suited for high-complexity subspecialty documentation compared to DeepScribe or Nuance
- Note customization is more limited at lower price tiers
- Support resources are lighter than enterprise-grade vendors
Best for: Solo physicians, independent practitioners, and small practices seeking immediate time savings at an accessible price point, without requiring IT infrastructure or long-term contracts.
7. Augmedix
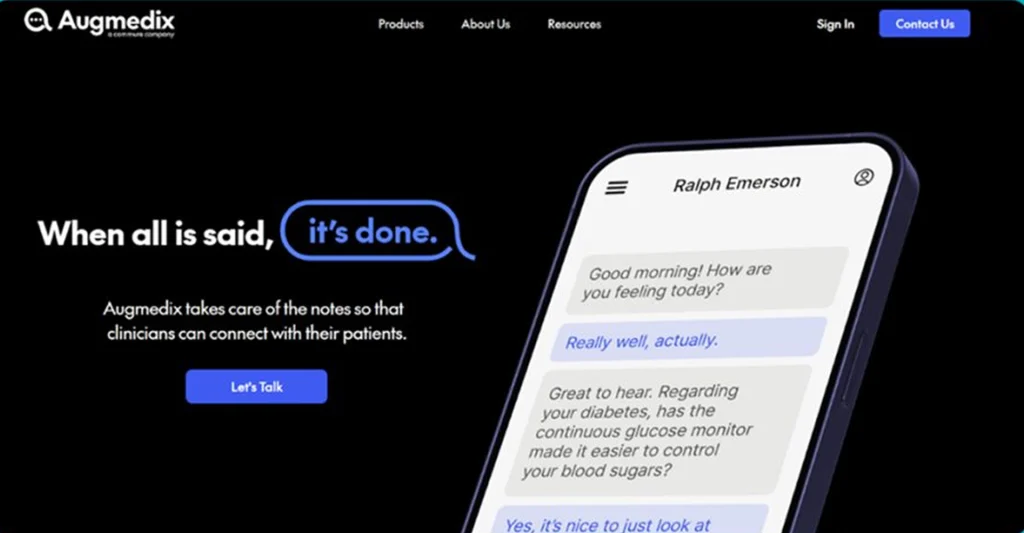
Augmedix takes a differentiated approach to AI medical documentation by combining ambient AI with human medical documentation specialists — creating a hybrid model that many physicians argue delivers the highest possible note accuracy, particularly in complex or high-ambiguity clinical situations. The Augmedix platform streams physician-patient encounters through a smart glass or mobile device to remote documentation specialists who, augmented by AI, produce structured clinical notes in real time. Acquired by Commure in 2023, Augmedix now serves some of the largest health systems in the United States, including HCA Healthcare. For any organization where documentation accuracy is non-negotiable, Augmedix’s human-in-the-loop approach provides a meaningful quality backstop.
- Star Rating: 4.2 / 5
- Target Audience: Health systems and practices seeking a hybrid human-AI documentation model for maximum accuracy.
Key Features:
- Hybrid AI + human documentation model — remote medical documentation specialists review and finalize AI-generated notes
- Ambient streaming via mobile device or smart glass — completely hands-free during encounters
- Real-time note delivery — completed notes typically available before the patient leaves the room
- Epic and Oracle Cerner native integrations; supports major EHR platforms
- Augmedix Go: AI-only, lower-cost tier for practices not requiring human review
- Works across all major specialties including emergency medicine, surgery, and primary care
- HIPAA-compliant with BAA, SOC 2 Type II, HITRUST certification
Pricing: Augmedix (full hybrid service): $800+/provider/month. Augmedix Go (AI-only): custom pricing available.
Pros:
- Human-in-the-loop backstop provides the highest practical note accuracy available
- Real-time note delivery improves clinical workflow and reduces end-of-day charting
- Ideal for emergency medicine, surgery, and high-acuity environments
- HITRUST certification offers the strongest compliance posture among AI scribe providers
- Augmedix Go tier provides a more affordable entry point with pure AI documentation
Cons:
- Highest price point for the full hybrid service, making it inaccessible for small practices
- Human-review component introduces slight privacy complexity that some institutions carefully evaluate
- Dependency on internet connectivity for real-time streaming
- Augmedix Go (AI-only) is less differentiated from pure-AI competitors at its price point
Best for: Health systems, large multi-specialty groups, and emergency or surgical departments where the cost of a documentation error is high and maximum note accuracy justifies premium pricing.
8. Heidi Health
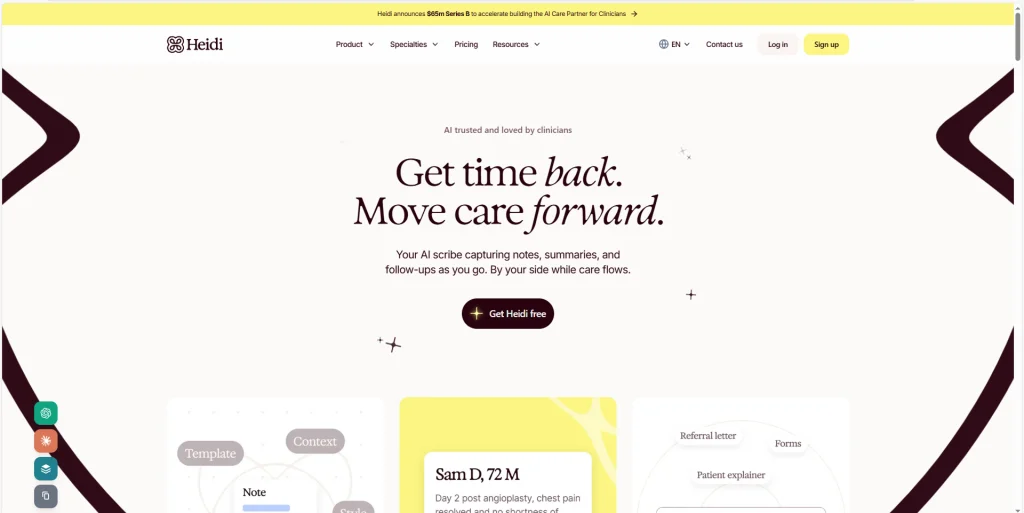
Heidi Health has built a devoted following among international and independent physicians by focusing relentlessly on ease of use, fast onboarding, and an accessible freemium pricing model. Originally launched in Australia and now serving physicians in the US, UK, Canada, and globally, Heidi Health positions itself as the AI scribe that “just works” — with no complex setup, no EHR dependency, and no lengthy trial required. The platform’s AI generates structured clinical notes from recorded encounters in under 30 seconds, supports custom templates and shorthand commands, and offers a free tier that allows physicians to evaluate the tool with real patients before committing.
- Star Rating: 4.3 / 5
- Target Audience: Independent physicians, small clinics, and telehealth providers worldwide.
Key Features:
- Free tier available — full-featured access with limited monthly note volume
- Ultra-fast note generation (under 30 seconds for standard encounter documentation)
- Custom template builder allowing physicians to define note structure for their specialty
- Supports general practice, family medicine, pediatrics, psychiatry, allied health, and more
- Global availability — HIPAA-compliant (US), GDPR-compliant (EU/UK), and AU privacy law compliant
- Works on mobile (iOS/Android) and web browser — no EHR installation required
- Push to any EHR via copy-paste; API integration available for tech-forward practices
Pricing: Free tier (limited notes/month); $70/month (Pro); $110/month (Pro Plus).
Pros:
- Free tier allows genuine risk-free evaluation with real patient encounters
- Fastest onboarding of any platform — most physicians are generating notes within 5 minutes
- Custom template builder gives practices strong control over note format
- Global compliance (HIPAA, GDPR, AU) — ideal for international clinicians or multinational practices
- Exceptional value for small practices and independent clinicians
Cons:
- No native EHR integration in core tiers — requires copy-paste workflow
- Free tier limitations may not be sufficient for high-volume practices
- Less enterprise-grade than Nuance, Abridge, or Ambience for complex health system deployments
- Clinical accuracy in highly complex or subspecialty-specific encounters may lag behind DeepScribe
Best for: Independent physicians, international clinicians, telehealth providers, and small clinics that want a reliable, affordable ambient scribe with a minimal learning curve and a risk-free free tier.
9. Nabla Copilot
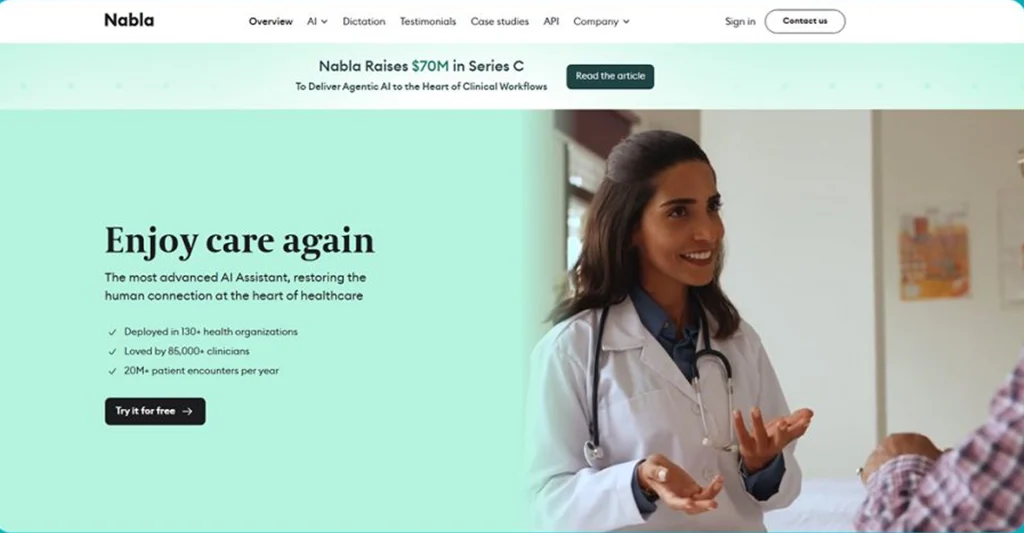
Nabla Copilot is a Paris-based ambient AI clinical documentation platform that has built a strong reputation in both the United States and European healthcare markets, supported by impressive venture backing and a focus on multilingual documentation and telemedicine workflow integration. The platform operates as an ambient overlay on top of telehealth and in-person encounters, generating structured clinical notes and consultation summaries in real time. Nabla is one of only a handful of AI scribes to offer native support for multiple European languages, making it an attractive choice for non-English-speaking healthcare environments. The platform integrates with major US EHRs (Epic, Cerner, athenahealth) and European EMR systems.
- Star Rating: 4.2 / 5
- Target Audience: Telehealth-heavy practices, multilingual clinical environments, and European healthcare organizations.
Key Features:
- Ambient AI documentation for in-person, video, and asynchronous telehealth encounters
- Multilingual support — works across English, French, Spanish, German, and other languages
- Integrates with Epic, Oracle Cerner, athenahealth, and European EMR platforms
- Generates SOAP notes, consultation summaries, referral letters, and after-visit instructions
- HIPAA-compliant (US) and GDPR-compliant (EU) — dual compliance architecture
- Team collaboration features including shared templates and group deployment tools
- Medical coding suggestions aligned with CPT and ICD-10 coding workflows
Pricing: Approximately $119/provider/month (individual); enterprise pricing for larger deployments.
Pros:
- Best-in-class multilingual ambient documentation — irreplaceable for non-English clinical environments
- Dual HIPAA/GDPR compliance makes it uniquely suited for cross-border and international practices
- Strong telehealth integration — one of the few AI scribes built equally for video and in-person encounters
- Accessible pricing compared to enterprise-only competitors
- Active product development with regular feature releases
Cons:
- Less brand recognition in the US enterprise market compared to Nuance or Abridge
- Multilingual strength is most valuable for non-English-speaking populations; less differentiating for English-only environments
- Some users report telehealth integration requires configuration for specific platforms
Best for: Telehealth-first practices, multilingual clinical environments, practices serving non-English-speaking patient populations, and healthcare organizations operating in both US and European markets.
10. DeepCura AI
DeepCura AI has earned a strong reputation on Capterra and G2 as one of the highest-rated AI medical scribe and clinical workflow platforms in its price category, offering a uniquely comprehensive feature set well below most enterprise competitors. Beyond ambient AI documentation, DeepCura functions as a full-stack clinical AI layer — combining ambient scribing, clinical decision support, order drafting, prior authorization, and patient triage AI into a single platform. Supporting 50+ medical specialties and integrating with all major EHR systems, DeepCura’s value proposition is compelling for any practice that wants to move beyond note generation toward broader AI-driven clinical workflow automation.
- Star Rating: 4.5 / 5
- Target Audience: Tech-forward practices and value-focused clinicians wanting a full-stack AI clinical workflow platform.
Key Features:
- Full-stack ambient AI: documentation + clinical decision support + order drafting + prior auth in one platform
- Supports 50+ specialties with fully customizable note templates and workflows
- Integrates with Epic, Cerner, athenahealth, eClinicalWorks, Kareo, and 30+ EHR platforms
- AI-generated draft orders, referral letters, and prior authorization requests
- Patient-facing triage AI that pre-screens patient intake before the encounter
- HIPAA-compliant, SOC 2 Type II, with BAA
- Highly customizable — practices can define their own note formats, AI instructions, and workflow automations
Pricing: $129/provider/month.
Pros:
- Exceptional value — full-stack AI clinical workflow platform at a fraction of enterprise pricing
- Highest-rated AI scribe on Capterra among comparable-priced platforms
- Broad EHR integration (30+ platforms) gives it wide deployment flexibility
- Full-stack approach (documentation + CDI + orders + prior auth) maximizes per-provider ROI
- Highly customizable — adapts to nearly any specialty’s workflow requirements
Cons:
- Less name recognition than Nuance, Abridge, or Suki among large health systems
- The full-stack feature set has a steeper learning curve than simpler ambient-only tools
- Some users report the AI decision support features require careful workflow configuration
- UI is more complex than consumer-grade tools like Freed or Heidi Health
Best for: Tech-forward practices and value-focused clinicians who want a full-stack AI clinical workflow platform — not just a note generator — at a competitive price point.
Comparison Table
| Platform | Best For | Price/Month | EHR Integration | Specialty Coverage | Rating |
|---|---|---|---|---|---|
| Nuance DAX Copilot | Large health systems | ~$369–$444 | 200+ EHRs (Epic native) | 20+ specialties | 4.5 / 5 |
| Abridge | Epic-based systems | ~$208 | Epic (native), Cerner | 50+ specialties | 4.5 / 5 |
| Ambience Healthcare | Enterprise clinical intelligence | Custom ($400–600+) | Epic, Cerner | 100+ specialties | 4.4 / 5 |
| Freed AI | Solo/small practice | $39–$119 | Any EHR (copy-paste + API) | 20+ specialties | 4.4 / 5 |
| DeepCura AI | Full-stack AI workflow | $129 | 30+ EHRs | 50+ specialties | 4.5 / 5 |
| Suki AI | Individual physicians | ~$299 | Epic, Oracle, Athena | Multi-specialty | 4.3 / 5 |
| DeepScribe | Complex specialties | ~$750 | Epic, Cerner, Athena, 40+ | 50+ specialties | 4.3 / 5 |
| Heidi Health | Independent/global clinicians | $70–$110 (Free tier) | Any EHR (copy-paste + API) | Multi-specialty | 4.3 / 5 |
| Nabla Copilot | Multilingual/telehealth | ~$119 | Epic, Cerner, Athena, EU EMRs | Multi-specialty | 4.2 / 5 |
| Augmedix | Human-AI hybrid accuracy | $800+ | Epic, Cerner | All specialties | 4.2 / 5 |
ExportCopy table
Specialty-Specific Guidance
Primary Care & Family Medicine
The priority is ease of use, speed, and affordability. Freed AI is the best budget option with its simple browser-based setup and adaptive note learning. Heidi Health excels on ease of use with its free tier and under-30-second note generation. DeepCura AI is the best value for practices wanting more than just a note generator. Sunoh.ai is ideal for high-volume clinics seeing 20+ patients per day where rapid note turnaround is critical.
Internal Medicine & Hospital Medicine
Complex multi-problem encounters and tight Epic integration requirements make enterprise-grade tools the best fit. Nuance DAX Copilot and Abridge are the top choices for hospitalists, with Abridge’s Epic-native workflow and 28-language support being particularly valuable in large academic centers. Ambience Healthcare adds CDI and coding support that can meaningfully improve hospitalist billing accuracy.
Surgery & Emergency Medicine
High-acuity, fast-paced encounters with complex procedural documentation benefit from Augmedix‘s human-in-the-loop accuracy model, particularly in environments where documentation errors have direct patient safety implications. Nuance DAX Copilot is the other primary choice for high-volume ED settings with existing Epic infrastructure.
Oncology, Cardiology & Complex Subspecialties
These specialties demand the highest clinical accuracy in note generation — terminology nuances, treatment plan documentation, and coding accuracy are non-negotiable. DeepScribe‘s multi-layer AI pipeline and Ambience Healthcare‘s CDI integration make them the top picks. Both are purpose-built for the documentation complexity that subspecialty care demands.
Psychiatry & Behavioral Health
Behavioral health documentation is highly sensitive and stylistically different — more narrative than SOAP-structured. Nabla Copilot and Heidi Health offer customizable note formats that accommodate the narrative style of psychiatric documentation, along with strong HIPAA compliance for sensitive mental health records. SimplePractice users will find Nabla’s integration particularly clean.
Telehealth-First and Multi-Site Practices
The best telehealth-native AI scribes must work cleanly on video platforms and support remote and in-person documentation in the same workflow. Nabla Copilot‘s telehealth-native architecture, Heidi Health‘s platform-agnostic browser-based approach, and Freed AI‘s flexible interface are all strong options for practices operating primarily or exclusively through virtual care.
FAQ Section
What is an AI medical scribe, and how is it different from traditional voice dictation?
An AI medical scribe is a tool that uses ambient artificial intelligence to listen to a natural conversation between a physician and a patient, then automatically generates a structured clinical note. This is fundamentally different from traditional voice dictation software (like Dragon Medical), which required a physician to actively speak commands and dictate sentences in a structured format. Ambient AI works passively in the background, understanding context, identifying speakers, and converting conversational dialogue into a professional-grade SOAP note without requiring the clinician to change their natural workflow.
Is ambient AI documentation HIPAA-compliant?
Yes. All leading AI medical scribe platforms are HIPAA-compliant and provide a Business Associate Agreement (BAA) to covered entities. These companies employ enterprise-grade security measures, including end-to-end encryption for all data in transit and at rest. Many also hold advanced security certifications like SOC 2 Type II or HITRUST, ensuring that patient data is handled according to the strictest privacy and security standards.
How long does it take to onboard an AI medical scribe?
Onboarding time varies significantly by platform. Simple, browser-based tools like Freed AI or Heidi Health can be set up in under 10 minutes with no IT support required. Enterprise-level platforms with deep EHR integrations, such as Nuance DAX Copilot or Ambience Healthcare, typically require a more involved, IT-led implementation process that can take several weeks to a few months to fully deploy across a health system.
Can AI medical scribes integrate with my existing EHR?
Yes, integration capabilities range from simple to deeply embedded. Many platforms offer a universal “copy-paste” workflow that works with any browser-based EHR. Others provide API-based integrations that push notes directly into dozens of major EHRs. The most advanced platforms, such as Nuance DAX Copilot and Abridge, offer native integrations that operate directly inside the Epic workflow for a seamless, hands-free experience.
Will AI-generated notes require editing before they go into the patient chart?
Yes. AI-generated notes should always be considered a “draft” that requires final review and sign-off by the clinician. While the accuracy of top-tier platforms can exceed 99% for common encounters, the physician is ultimately responsible for the final content of the medical record. The goal of an AI scribe is to eliminate 80–90% of the manual documentation work, leaving the clinician with a quick review and edit process rather than starting from scratch.
Are AI medical scribes accurate enough for complex specialties?
Yes, several platforms are specifically designed for the nuances of high-complexity specialties. Tools like DeepScribe and Ambience Healthcare use specialty-tuned AI models and advanced clinical knowledge graphs to achieve high accuracy in fields like oncology, cardiology, and neurology. For environments where absolute accuracy is paramount, hybrid models like Augmedix add a layer of human quality assurance to the AI-generated draft.
What is the ROI of an AI medical scribe for a typical practice?
The ROI is multifaceted. The most direct benefit comes from time savings, with physicians reporting they save between one to three hours per day on documentation, reducing “pajama time” and burnout. This reclaimed time can be used to see more patients, increasing revenue, or to restore work-life balance. Secondary ROI comes from improved coding accuracy, reduced claim denials, and better patient engagement from more attentive, less-distracted encounters.
What should I look for when choosing an AI medical scribe for my practice?
The best choice depends on your practice’s specific needs. Key factors to consider include your specialty, your EHR system, your budget, and your practice size. For solo or small practices, affordability and ease of use — Freed AI and Heidi Health — are often the top priorities. For large health systems, deep EHR integration and enterprise-grade security — Nuance DAX and Abridge — are critical. For high-complexity specialists, clinical accuracy — DeepScribe and Ambience — is non-negotiable.
Choose the Right Platform
The AI medical scribe landscape of 2025 is mature, robust, and delivering on its promise to combat physician burnout. What was once an experimental technology has become a standard of care, with adoption accelerating across every type of healthcare organization, from solo practices to the nation’s largest health systems. By automating the laborious process of clinical documentation, these tools save physicians hours each day, improve the quality of patient interactions, and restore a crucial measure of work-life balance to a profession in crisis.
Choosing the right platform is a matter of matching the tool to the clinical context. Large enterprise health systems should focus their evaluations on Nuance DAX Copilot, Abridge, or Ambience Healthcare for their deep EHR integration and enterprise-grade support. Mid-size multi-specialty groups will find compelling options in Suki AI, DeepScribe, or the full-stack DeepCura AI platform. For solo and independent practices, Freed AI, Heidi Health, and DeepCura AI offer the best combination of value, flexibility, and ease of use. Complex subspecialists should prioritize the clinical accuracy of DeepScribe and Ambience, while telehealth-heavy or multilingual practices will be best served by Nabla Copilot.
The documentation burden is real, the technology is proven, and the ROI is no longer theoretical. Every physician still spending evenings and weekends catching up on charting owes it to themselves, their families, and their patients to evaluate an AI medical scribe in 2025. Request demos from two to three platforms that match your practice profile, take advantage of the free tiers offered by Heidi Health and Freed AI, and measure the time you reclaim in the first 30 days.